Redefining Immunization: Not Just a Shot in the Arm
The Evergreen State College (Anderson); Morehouse School of Medicine (Wilson, Moon); The Lloyd Best Institute of the West Indies, Tunapuna (Kanem); Malango Traditional Healers Association (Diop); PROMETRA International (Gbodossou)
"...explanations of underimmunization have focused on ignorance, misinformation, and a need to educate populations on its importance, but trusted sources of local knowledge and leadership may also affect community levels of trust, distrust, comfort or anxiety related to Western-based immunization practices..."
In Sub-Saharan Africa, traditional health practitioners (THPs) - healers and birth attendants - play a major role in providing health care and health education, particularly in rural areas where Western health care is unavailable. "Their ancestral community roots and intimate, direct experience of poverty, inequity, and disease have earned them a wide and respectful audience as well as an in-depth knowledge of the culture...". The project Immunization Advocacy: Saving Lives of Africa’s Children, funded by the Bill and Melinda Gates Foundation, was carried out in Benin, Nigeria, and Senegal with THPs and other community-based leaders to gain insight into their basic knowledge, attitudes, and perceptions of immunisations, the associated infrastructures, and their overall perceptions of preventive health measures, particularly beliefs and practices that may affect infant well-being. This research paper presents the results from the Senegal study, which surveyed 696 THPs involved in community culture, rites, education, and health.
Some context is provided. The national infant mortality and under-5 mortality rates are 45 and 55 per 1000 live births (Gavi, 2014). The literacy rate is low (39.3%), particularly among young women, who are most commonly mothers of vaccine-age children. The country has free and obligatory vaccination for every child, infectious and parasitic diseases are dominant causes of disease and death, and vaccine coverage has been estimated at 80% for measles, 85% for polio, and 89% for diphtheria, pertussis (whooping cough), and tetanus (DPT3) in 2013.
Three regions were chosen for survey in this study to provide settings that included urban neighbourhoods (Dakar), a centre of Islamic religion (Diourbel), and Fatick, where endogenous culture and religion are very important. The study was conducted between November 2009 and November 2011 in partnership with the Association of Islamic Charities and the Malango Association of Traditional Healers, an organisation recognised by the Senegal government. Focus groups were held using semi-structured interviews to provide insight on questionnaire development. In contrast with the (Western) biomedical definition of immunisation, the traditional healers and community leaders' definition included all of the practices (possibly including but not limited to vaccination) that support wellness and prevent illness through the support of the human ability to stay healthy and avoid disease. This definition of immunisation was integrated into the questionnaires and interviews, and it allowed the study to explore ways in which traditional health-promoting practices are congruent with biomedical belief systems and ways that they differ.
Results of the study in Senegal show that although knowledge about vaccination is high among THPs, their perceptions of vaccines may hinder the acceptance of vaccines in their communities. Specifically, 99% of those who were surveyed stated they were familiar with vaccination, 2.3% reported vaccinating their children or grandchildren, and about 90% acknowledged that vaccination provides protection against diseases (see details in Table 2). Among the participants, 72% thought that infant vaccination during the first 6 months is acceptable. However, only 27% acknowledged participating in vaccination campaigns. Concerns can be divided into the 4 broad categories of practical/material and logistical constraints (90% cited lack of resources as a concern), concerns about potential adverse health effects, cultural considerations (e.g., beliefs about unwise or forbidden behaviour and perceptions circulating in the community about the effects of vaccination on fertility), and perceptions that the biomedical health care providers lack competency and have not considered the importance of community-based leaders in vaccine campaigns.
The study participants had clear ideas about ways to improve THP support for vaccinations. The THPs indicated that they want to be involved in the immunisation advocacy or support processes (see Table 3). In addition, they emphasised that their perceptions on immunisation and vaccination such as taboos, endogenous knowledge, beliefs, and economic and cultural factors should be considered when making decisions on vaccination that affect their communities. THPs suggested there is the need for increased accessibility of vaccination points in communities. Results emphasising the importance of THP involvement in vaccine-related interventions are confirmed in Table 4, where binary logistic regression, controlling for potential confounders such as age and gender, demonstrates that THPs who are full-time healers are most likely to believe that biomedical immunisation is ineffective (OR= 3.78, 95% CI [1.62, 8.84]), and the perception of THP noninvolvement in vaccine planning and interventions was associated with the perception that vaccines are ineffective (OR = 10.57, 95% CI [2.94, 37.95]). This association was also statistically significant, unlike any associations related to rumors of fertility reduction or cultural taboos (see Table 4).
In the discussion section, the authors note that many of the results presented in this study are consistent with other similar studies in that poverty, access, perceived quality, potential side effects, and characteristics of health worker behaviour are directly related to perceptions related to vaccine use. They cite several studies, such as those stressing that, before a routine national immunisation programme is introduced, careful consideration should be taken on how best to facilitate trust between the communities and the healthcare system in a sustainable way that does not overburden already stretched resources and personnel. However, in addition, they outline some implications of their study results for national health ministries and all hoping to increase vaccination rates:
- THPs can act as advocates for vaccination programmes provided that they are involved in planning and are assured that their cultures and belief systems will be respected. Despite their concerns about vaccine effectiveness and the extremely low percentage of THPs who immunise their own children or grandchildren, most THPs surveyed know about vaccination, believe that it has protective effects, and are comfortable with infant vaccination that starts at less than 6 months of age.
- The THPs' comprehensive definition of disease prevention includes nutritional support and traditional practices for pregnant women and infants. Some of these beliefs, such as the importance of a varied diet, are consistent with Western perceptions of healthy behaviours. "The THPs understand the multiple factors responsible for poor child health in their communities, and they recognize the overwhelming importance of malnutrition and poverty as health risk factors for women and children. Their perceptions are completely congruent with public health evidence." Some other parts of their belief system are not a part of Western biomedicine but are not in direct competition with biomedical beliefs and may easily coexist with them.
- The results of this study call for a culture-centred, culturally embedded approach to health communication that recognises the central importance of endogenous culture, that values the definition of health and prevention encompassed within the THP definition of immunisation, and that uses this definition as the working description of what immunisation programmes should provide.
- "THPs, who deliver the majority of front line primary care in many parts of Sub-Saharan Africa, must be directly involved in defining the conceptual framework of health, and in developing preventive health policy priorities that include but are not limited to vaccines. Governmental health institutions must accept them as primary sources of health education and as experts in communication substance and strategy."
- "[P]olicymakers must realize that people understand the difference between the comprehensive support needed to improve maternal-infant health in Africa and the limited tools that are currently offered. THPs' knowledge, attitudes, and perceptions in the context of this study confirm that healers can and must play a leadership role bridging the gap between the lofty goals of health for all and the existing health conditions that still limit the health and wellbeing of Africa."
In short: "Effective educational programs that involve THPs in vaccine campaigns from inception, that address their perceptions and integrate their cultural belief systems into vaccine advocacy programs in a culture-centered manner, and that recognise and respect the importance of comprehensive primary health care will be necessary to improve essential vaccine coverage in this population."
Editor's note: This paper has been published as part of a United States Agency for International Development (USAID)-funded initiative to increase the number of peer-reviewed papers on routine and polio communication and to ensure that academics from a range of countries, including those facing the greatest polio and routine immunisation challenges, are supported in getting their research peer reviewed, published, and widely disseminated through The CI and the new journal Global Health Communication.
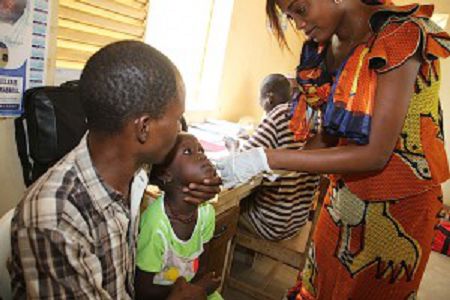
Global Health Communication, 1:1, 1-9, DOI: 10.1080/23762004.2016.1161416. Image credit: PATH/Fatou Kande
- Log in to post comments












































